Digestive Health Specialists, PA is here to help if you, or someone you know, would like more information, or if you are experiencing any digestive health symptoms and would like further evaluation. Feel free to give us a call at 336-768-6211 or fill the form below.
Top 5 Digestive Problems that Affect Men
June is Men’s Health Month and we want to bring attention to gastrointestinal conditions that affect a large number of men.
Belching, Bloating, and Flatulence
Belching, bloating, and flatulence occurs when swallowed air is accumulated in the stomach. The air can either be belched out or can be passed out of the stomach into the small intestine and then passed as rectal gas (flatus).
We all swallow air during the process of eating. The most common reasons for excess swallowing are:
- Sucking on hard candies or chewing gum
- Drinking carbonated beverages, such as soda or beer
- Anxiety
- Poorly fitting dentures
- Chronic postnasal “drip”
To decrease symptoms, patients should eliminate carbonated beverages such as soda and beer; foods such as cauliflower, broccoli, cabbage, beans, and bran; milk, and other dairy foods. Lactaid milk or non-dairy milk such as soy or almond milk can be used. Chewing gum and sucking on hard candies should be avoided. Sugar-free gum and hard candies should be avoided as they may have mannitol or sorbitol as sweeteners which can cause flatulence. To ensure that only potentially symptom causing foods are eliminated without resulting in marked dietary restrictions, patients should eliminate food items one by one and keep a symptom diary.
Acid Reflux and GERD
Gastroesophageal reflux is a physical condition in which acid from the stomach flows backward up into the esophagus. People will experience heartburn symptoms when excessive amounts of acid reflux into the esophagus. However, frequent heartburn (two or more times a week), food sticking, blood, or weight loss may be associated with a more severe problem known as gastroesophageal reflux disease or GERD.
In many cases, doctors find that infrequent heartburn can be controlled by lifestyle modifications and proper use of over-the-counter medicines.
Lifestyle Modifications:
- Avoid foods and beverages that contribute to heartburn: chocolate, coffee, peppermint, greasy or spicy foods, tomato products, and alcoholic beverages.
- Stop smoking. Tobacco inhibits saliva, which is the body’s major buffer. Tobacco may also stimulate stomach acid production and relax the muscle between the esophagus and the stomach, permitting acid reflux to occur.
- Reduce weight if too heavy.
- Do not eat 2-3 hours before sleep.
- For infrequent episodes of heartburn, take an over-the-counter antacid or an H2 blocker, some of which are now available without a prescription.
Constipation
For many people, constipation means too much straining with bowel movements, the passage of small hard stools, or a sense that they have not completely emptied their bowels. Constipation most commonly occurs when the waste (stool) that forms after food is digested moves too slowly (slow transit) as it passes through the digestive tract. Dehydration, changes in diet and activity, and certain drugs are common reasons for the slow transit of stool. When stool moves slowly, too much water is absorbed from the stool, and it becomes hard and dry.
Several options are available for treating constipation.
- Increasing the intake of fluids and fiber
- Vegetables, fruit (especially prunes), whole-grain bread, and high-fiber cereals
- Bran – although it may cause excessive gas and bloating.
To work well, fiber should be consumed with plenty of fluids.
Laxatives and stool softeners are sometimes needed if changes in diet are insufficient. Most laxatives are safe for long-term uses, if used appropriately.
When the stool is impacted, tap water enemas are commonly used. If enemas fail to work, a health care practitioner may need to remove the stool manually using a gloved finger. The person is then sometimes asked to drink a solution containing dissolved salts and polyethylene glycol, which cleanses the digestive tract.
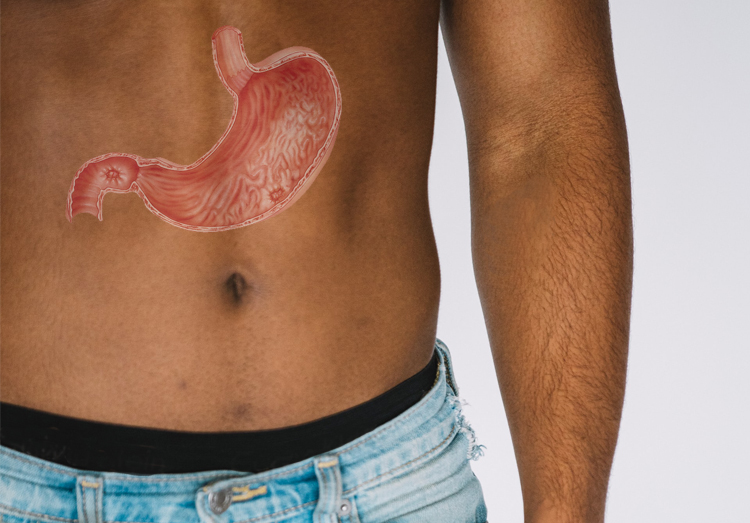
Peptic Ulcers
An “ulcer” is an open sore. The word “peptic” means that the cause of the problem is due to acid. The two most common types of peptic ulcers are called “gastric ulcers” and “duodenal ulcers”. These names refer to the location where the ulcer is found. Gastric ulcers are located in the stomach, while duodenal ulcers are found at the beginning of the small intestine known as the duodenum. A person may have both gastric and duodenal ulcers at the same time.
The two most important causes of ulcers are infection with Helicobacter pylori and a group of medications known as NSAIDs.
- Helicobacter pylori (also called H. pylori or “HP) is a bacterium that lives in the stomach of infected people.
- NSAIDs (Non-Steroidal Anti-Inflammatory Drugs) are a group of medications typically used to treat pain.
The way that ulcers are treated depends on a number of features. Nearly all peptic ulcers will be treated with a proton pump inhibitor (PPI). PPIs are powerful acid-blocking drugs that can be taken as a pill or given in an IV. Sometimes duodenal ulcers (not gastric ulcers) will be treated with H2 blockers. H2 blockers are another type of acid-reducing medication. If the person is infected with H. pylori this infection should be treated. Completing the full dose of antibiotics is very important. Just as important, is making sure that the infection is gone.
Most ulcers can be treated and will heal.
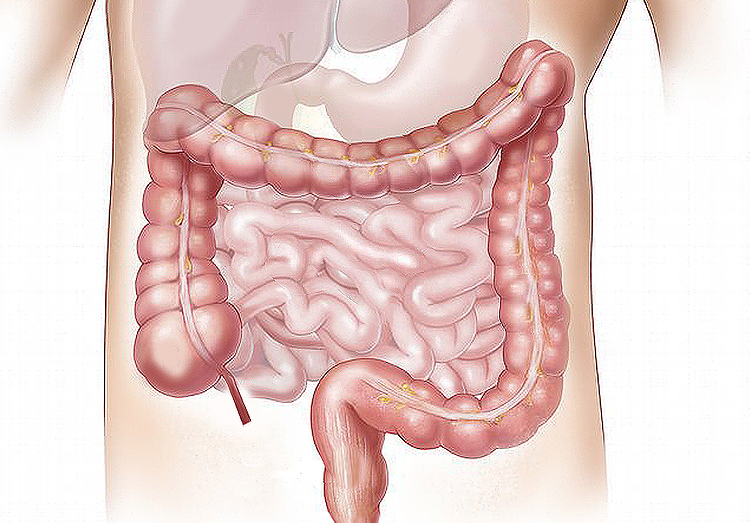
Colon Cancer
Colorectal (large bowel) cancer is a disease in which malignant (cancer) cells form in the inner lining of the colon or rectum. Most colon and rectal cancers originate from benign wart-like growths on the inner lining of the colon or rectum called polyps. Not all polyps have the potential to transform into cancer. Those that do have the potential are called adenomas. It takes more than 10 years in most cases for an adenoma to develop into cancer. This is why some colon cancer prevention tests are effective even if done at 10-year intervals. This 10-year interval is too long, in some cases, such as in persons with ulcerative colitis or Crohn’s colitis, and in persons with a strong family history of colorectal cancer or adenomas.
Preferred Colorectal Cancer Prevention Test: Colonoscopy
Colonoscopy every 10 years is the preferred colorectal cancer prevention test. For normal risk individuals, the American College of Gastroenterology recommends colonoscopy beginning at age 50, and age 45 for African Americans.
The information in this article was summarized from the American College of Gastroenterology website: https://gi.org/
Do you suffer from any of the conditions listed here? Let us know.