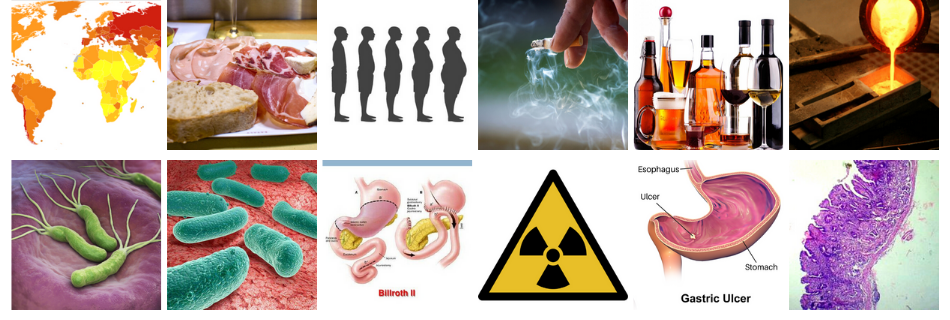
Stomach Cancer and Your Risk Factors
Gastric cancer is one of the most common cancers worldwide. Before the 1980s, it was the leading cause of cancer death. Over the last 40 years, there has been a decline in the incidence, for unexplained reasons.
Risk Factors
- Race – East Asians, Andean South Americans, and Eastern Europeans are at the highest risk for gastric cancer.
- Diet – Diets high in salt and preserved foods such as cured meats, nitrate-containing foods, salted fish and vegetables can increase the risk of gastric cancer.
- Obesity – Obesity defined as a BMI>25 is associated with an increased risk.
- Smoking – Smoking, as you would imagine, is related to gastric cancer.
- Alcohol – There is no association between alcohol and gastric cancer.
- Occupational exposures – Occupations that involve coal, tin, metal processing, and rubber manufacturing can increase the risk.
- Helicobacter pylori – Helicobacter pylori is a definite carcinogen. It is a very common bacteria that colonize in the stomach and can remain asymptomatic for many years.
- Epstein-Barr virus – EBV or Epstein-Barr virus is associated with nasopharyngeal cancer and gastric cancer.
- Gastric surgery – There is an increased risk of gastric cancer after gastric surgery such as a Billroth I and II procedure. There is no data between gastric cancer and gastric bypass surgery.
- Abdominal radiation exposure – Patients who may have had other malignancies requiring radiation to the abdomen are at increased risk.
- Ulcers – Gastric ulcers increase the risk of gastric cancer.
- Atrophic gastritis (pernicious anemia) – Atrophic gastritis, a condition where gastric cells become nonfunctioning, can lead to B12 deficiency and gastric cancer
Most gastric cancers are sporadic. Only a very small percentage are familial or hereditary. Environmental risk factors are more likely involved than genetics.
Symptoms:
Common symptoms are:
- Weight loss
- Abdominal pain
- Early satiety
- Bleeding
- Anemia
- Dysphagia (trouble swallowing).
Unfortunately, patients are typically asymptomatic. Most patients, when they present with symptoms, are already at an advanced stage. At an advanced stage, the disease is incurable when diagnosed. Early detection is not always possible, but when it does occur, a cure can be achieved.
Diagnosis:
Upper endoscopy is the preferred diagnostic test for a patient in whom gastric cancer is suspected. With this test, the tumor can be seen and biopsies can be obtained. Barium x-rays are the alternative, but false-negative studies can occur in up to 50% of cases. Abnormal x-rays will require a follow up diagnostic upper endoscopy.
Fruits, vegetables, and fiber are probably protective against gastric cancer. There have also been beneficial associations linked with NSAID use and certain reproductive hormones.
Screening for gastric cancer is controversial. It can be performed with upper endoscopy and barium x-rays. In high-risk patients in Asia, an endoscopy is performed every 2-3 years after the age of 40 in Korea and 50 in Japan. Patients with gastric adenomas, pernicious anemia, gastric intestinal metaplasia, familial adenomatous polyposis, Lynch syndrome, Peutz-Jeghers syndrome, and juvenile polyposis syndrome also benefit from screening procedures.
Do you feel you are at risk for gastric cancer? Let us know why below.

Board-certified gastroenterologist at Digestive Health Specialists.
He works at our Advance and Kernersville clinics.
Learn more about him here: https://digestivehealth.ws/provider/christopher-t-jue/
Digestive Health Specialists, PA is here to help if you, or someone you know, would like more information, or if you are experiencing any digestive health symptoms and would like further evaluation. Feel free to give us a call at 336-768-6211 or fill the form below.